Covid-19 isn’t going away soon. Two recent studies mapped out the possible shapes of its trajectory.

By Siobhan Roberts – May 8, 2020
By now we know — contrary to false predictions — that the novel coronavirus will be with us for a rather long time.
“Exactly how long remains to be seen,” said Marc Lipsitch, an infectious disease epidemiologist at Harvard’s T.H. Chan School of Public Health. “It’s going to be a matter of managing it over months to a couple of years. It’s not a matter of getting past the peak, as some people seem to believe.”
A single round of social distancing — closing schools and workplaces, limiting the sizes of gatherings, lockdowns of varying intensities and durations — will not be sufficient in the long term.
In the interest of managing our expectations and governing ourselves accordingly, it might be helpful, for our pandemic state of mind, to envision this predicament — existentially, at least — as a soliton wave: a wave that just keeps rolling and rolling, carrying on under its own power for a great distance.
The Scottish engineer and naval architect John Scott Russell first spotted a soliton in 1834 as it traveled along the Union Canal. He followed on horseback and, as he wrote in his “Report on Waves,” overtook it rolling along at about eight miles an hour, at thirty feet long and a foot or so in height. “Its height gradually diminished, and after a chase of one or two miles I lost it in the windings of the channel.”

The pandemic wave, similarly, will be with us for the foreseeable future before it diminishes. But, depending on one’s geographic location and the policies in place, it will exhibit variegated dimensions and dynamics traveling through time and space.
“There is an analogy between weather forecasting and disease modeling,” Dr. Lipsitch said. Both, he noted, are simple mathematical descriptions of how a system works: drawing upon physics and chemistry in the case of meteorology; and on behavior, virology and epidemiology in the case of infectious-disease modeling. Of course, he said, “we can’t change the weather.” But we can change the course of the pandemic — with our behavior, by balancing and coordinating psychological, sociological, economic and political factors.
Dr. Lipsitch is a co-author of two recent analyses — one from the Center for Infectious Disease Research and Policy at the University of Minnesota, the other from the Chan School published in Science — that describe a variety of shapes the pandemic wave might take in the coming months.
The Minnesota study describes three possibilities:
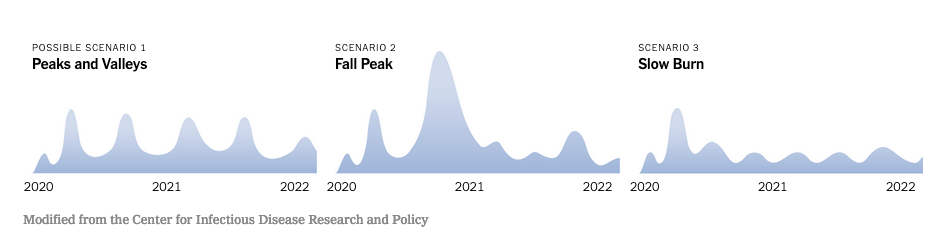
Scenario No. 1 depicts an initial wave of cases — the current one — followed by a consistently bumpy ride of “peaks and valleys” that will gradually diminish over a year or two.
Scenario No. 2 supposes that the current wave will be followed by a larger “fall peak,” or perhaps a winter peak, with subsequent smaller waves thereafter, similar to what transpired during the 1918-1919 flu pandemic.
Scenario No. 3 shows an intense spring peak followed by a “slow burn” with less-pronounced ups and downs.
The authors conclude that whichever reality materializes (assuming ongoing mitigation measures, as we await a vaccine), “we must be prepared for at least another 18 to 24 months of significant Covid-19 activity, with hot spots popping up periodically in diverse geographic areas.”
In the Science paper, the Harvard team — infectious-disease epidemiologist Yonatan Grad, his postdoctoral fellow Stephen Kissler, Dr. Lipsitch, his doctoral student Christine Tedijanto and their colleague Edward Goldstein — took a closer look at various scenarios by simulating the transmission dynamics using the latest Covid-19 data and data from related viruses.
The authors conveyed the results in a series of graphs — composed by Dr. Kissler and Ms. Tedijanto — that project a similarly wavy future characterized by peaks and valleys.
One figure from the paper, reinterpreted below, depicts possible scenarios (the details would differ geographically) and shows the red trajectory of Covid-19 infections in response to “intermittent social distancing” regimes represented by the blue bands.
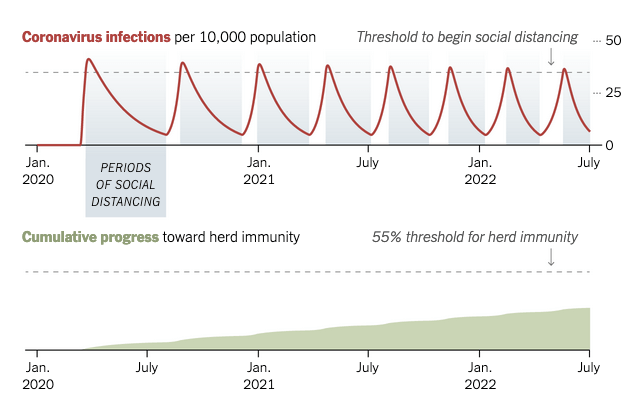
Social distancing is turned “on” when the number of Covid-19 cases reaches a certain prevalence in the population — for instance, 35 cases per 10,000, although the thresholds would be set locally, monitored with widespread testing. It is turned “off” when cases drop to a lower threshold, perhaps 5 cases per 10,000. Because critical cases that require hospitalization lag behind the general prevalence, this strategy aims to prevent the health care system from being overwhelmed.
The green graph represents the corresponding, if very gradual, increase in population immunity.
“The ‘herd immunity threshold’ in the model is 55 percent of the population, or the level of immunity that would be needed for the disease to stop spreading in the population without other measures,” Dr. Kissler said.
Another iteration shows the effects of seasonality — a slower spread of the virus during warmer months. Theoretically, seasonal effects allow for larger intervals between periods of social distancing.
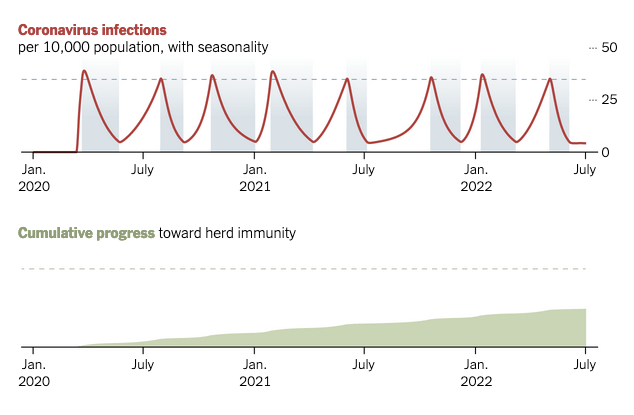
This year, however, the seasonal effects will likely be minimal, since a large proportion of the population will still be susceptible to the virus come summer. And there are other unknowns, since the underlying mechanisms of seasonality — such as temperature, humidity and school schedules — have been studied for some respiratory infections, like influenza, but not for coronaviruses. So, alas, we cannot depend on seasonality alone to stave off another outbreak over the coming summer months.
Yet another scenario takes into account not only seasonality but also a doubling of the critical-care capacity in hospitals. This, in turn, allows for social distancing to kick in at a higher threshold — say, at a prevalence of 70 cases per 10,000 — and for even longer breaks between social distancing periods:

What is clear overall is that a one-time social distancing effort will not be sufficient to control the epidemic in the long term, and that it will take a long time to reach herd immunity.
“This is because when we are successful in doing social distancing — so that we don’t overwhelm the health care system — fewer people get the infection, which is exactly the goal,” said Ms. Tedijanto. “But if infection leads to immunity, successful social distancing also means that more people remain susceptible to the disease. As a result, once we lift the social distancing measures, the virus will quite possibly spread again as easily as it did before the lockdowns.”
So, lacking a vaccine, our pandemic state of mind may persist well into 2021 or 2022 — which surprised even the experts.
“We anticipated a prolonged period of social distancing would be necessary, but didn’t initially realize that it could be this long,” Dr. Kissler said.